A Patient’s Guide to Tendonitis
Introduction
Chronic, or long-term, tendon problems are common. Tendon problems are especially common in people who play certain types of sports. Tendon problems account for almost 30 percent of all running injuries and 40 percent of all tennis injuries.
We use the term tendonitis, which means inflammation of the tendon, to refer to these chronic tendon problems. Doctors now know that the tendon does not always become inflamed when it is injured. Other changes in the tendon can cause tendon pain. However, tendonitis is still the most commonly used term.
This guide will help you understand
- how tendonitis develops
- how doctors diagnose the condition
- what can be done for tendonitis
Anatomy
Where does tendonitis develop?
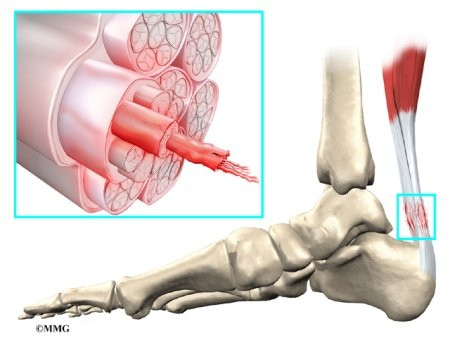
Tendons connect muscle to bone. A tendon is made of material called collagen. Collagen is a key building block of the body. Collagen is considered a connective tissue because it forms tough strands that are like the strands of a nylon rope. Like the strands in a rope, the strands of collagen line up. The more strands, and the better they line up, the stronger they are. The tendon is wrapped in a thin, slippery covering called the tendon sheath. The tendon sheath allows the tendon to slide easily against the tissues around it.
Many parts of the tendon can be injured. Tendon problems can involve the area where the tendon attaches to the bone, the tissue that surrounds the tendon (the tendon sheath), or the main tissues of the tendon. Doctors use different terms to refer to injuries of different parts of the tendon.
Tendon injuries can show up anywhere in your body. Doctors see tendonitis most often in certain sites.
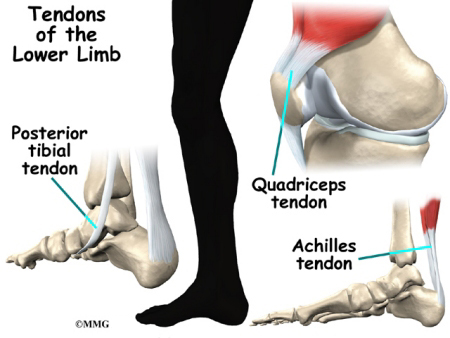
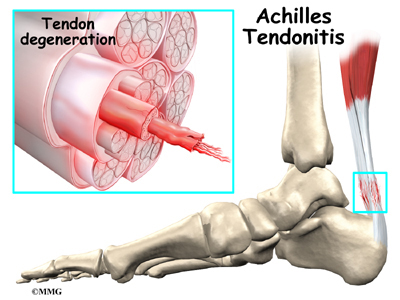
Achilles Tendonitis
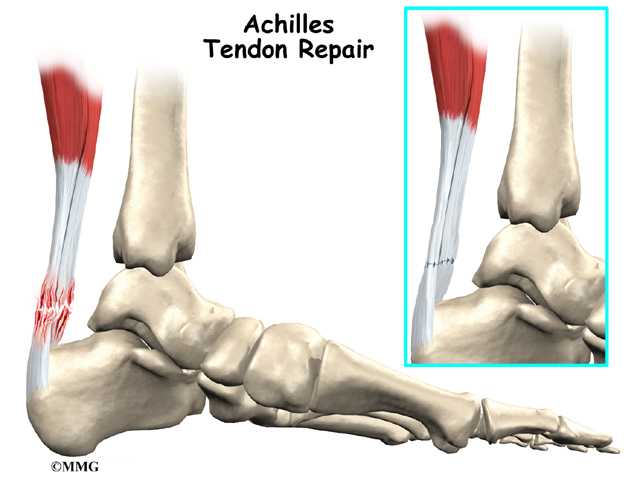
The tendon sheath, the tissues of the tendon, and the attachment to the bone can all become injured in the Achilles tendon, found in the lower leg. Damaged Achilles tendons carry a higher risk of rupturing because of the weight they bear while standing and walking.
Related Document: A Patient’s Guide to Achilles Tendon Problems
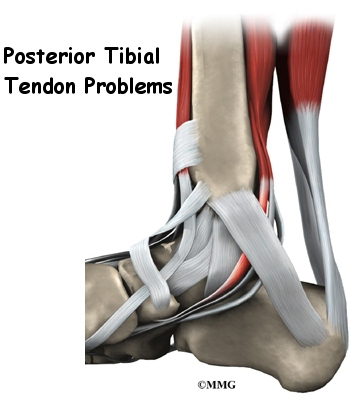
Posterior Tibial Tendonitis
Tendonitis along the inside edge of the ankle and into the instep of the foot is called posterior tibial tendonitis. It is usually caused by age-related degeneration. If this tendon breaks, it can cause the arch of the foot to become flat and painful.
Related Document: A Patient’s Guide to Posterior Tibial Tendon Problems
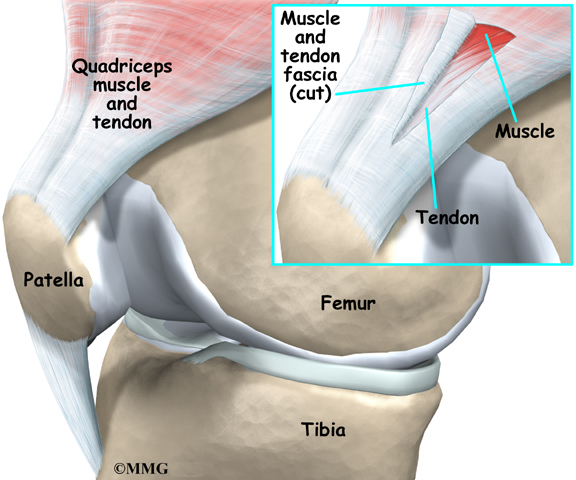
Patellar and Quadriceps Tendonitis
Problems in the tendons of the knee occur mostly in people whose exercise involves running or jumping. Patellar tendonitis is also called jumper’s knee.
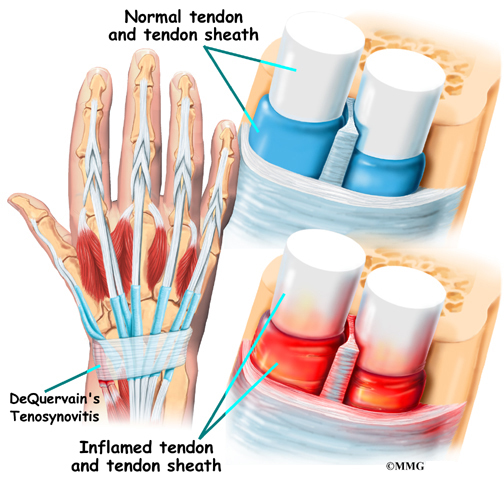
De Quervain’s Disease and Trigger Finger
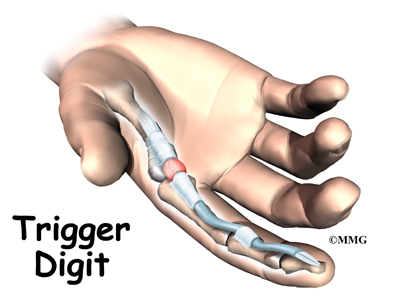
Tendon problems are common in the hand and wrist. De Quervain’s disease causes pain in the wrist just above the thumb. Trigger finger generally causes pain in the palm just below the knuckles, but it eventually causes problems with movement.
Related Document: A Patient’s Guide to De Quervain’s Tenosynovitis
Related Document: A Patient’s Guide to Trigger Finger and Trigger Thumb
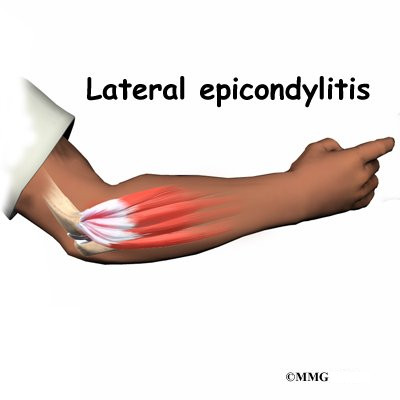
Lateral Epicondylitis
Lateral epicondylitis, also called tennis elbow, affects the area where the tendons of the elbow attach to bone on the outside of the elbow. It causes pain when using the wrist and hand.
Related Document: A Patient’s Guide to Lateral Epicondylitis
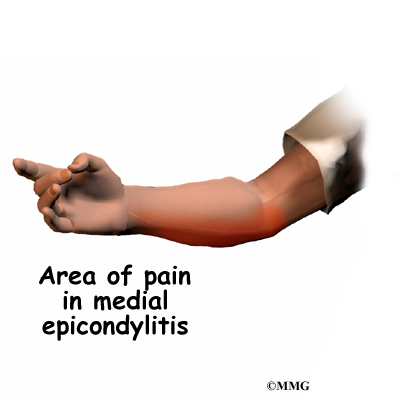
Medial Epicondylitis
Medial epicondylitis, also called Golfer’s elbow, affects the area where the tendons of the elbow attach to bone on the inside of the elbow. It causes pain when using the wrist and hand.
Related Document: A Patient’s Guide to Medial Epicondylitis
Rotator Cuff Tendonitis
Rotator cuff problems of the shoulder range from mild damage to complete tears. They can cause pain even when resting.
Related Document: A Patient’s Guide to Rotator Cuff Tears
Often, the muscles or other tissues of the joints become tight, misaligned, or weak around the area of tendon injury. Some of the pain and swelling of tendonitis may actually be in the surrounding tissues.
Causes
Why do I have this problem?
Doctors don’t know exactly what causes most tendon problems. They think that repetitive stress on the tendon is the most common cause. The tendon can be injured by the repetitive pounding of running and jumping, or by the stress caused by lifting heavy loads over and over again. Tendonitis usually builds up over weeks or months.
If the tendon is too damaged, or if it doesn’t get time to heal, the problem becomes chronic (long-lasting). In general, the heavier the load or the more often the stress is repeated, the more likely you are to develop tendonitis.
Too much stress on the tendons can be made worse by other factors. Lack of flexibility or weakness in your muscles can make tendonitis more likely. Shoes that don’t fit right, poor equipment, or incorrect technique can also increase your risk of tendon injury. Don’t underestimate the benefit of upgrading your equipment. The improved design of athletic shoes over the past few decades seems to have decreased tendon injuries.
Aging seems to cause tendon damage in some cases. As we age, the tissues of the tendon can break down, or degenerate. Age-related tendon problems do not seem to cause inflammation. The tendon material itself is more affected in these conditions and some surgeon’s refer to this type of tendon problem as tendonosis.
Some researchers think that a decreased blood supply to the tendons can cause the tendon damage in tendonosis. The decreased blood supply does not allow the tendon to get enough oxygen from the blood. This leads to a condition where the tendon degenerates. The collagen material that makes up the tendon actually becomes weaker and loses its nylon rope appearance. This type of degeneration has been noted in the rotator cuff around the shoulder, in the Achilles tendon in the heel and in the tendons of the elbow.
Many factors can work together to cause tendonitis. For instance, a woman in her forties who takes up running may have tendonitis caused jointly by the degeneration of aging and the mechanical stress of running.
Symptoms
What does tendonitis feel like?
Tendonitis causes pain. This is the primary symptom of tendonitis and tendonosis. The affected tendons are sometimes swollen. In some cases this swelling occurs from actual thickening of the tendon itself. In other cases the swelling comes from thickening or swelling of the tendon sheath. Tendon problems often cause pain after resting, such as when you first get up in the morning. This pain usually goes away within minutes, or even seconds.
The pain or swelling in your tendon may make your joint hard to move. Some types of tendon problems cause crepitus, a crackling feeling when the joint moves. In rare instances the weakened tendon may actually rupture, or break, with a sudden force. This may require surgery to repair.
Diagnosis
How do doctors identify tendonitis?
Your doctor will take a detailed medical history, including many questions about your activities, your job, and your symptoms. Your doctor will also physically examine the sore area. The probing and movement may cause pain, but it is important for your doctor to know exactly where it hurts.
X-rays do not usually show tendon damage. Your doctor may still ask you to get an X-ray or another imaging test to rule out other problems. Sometimes tendon injuries and other joint or muscle problems occur together. In some cases your doctor may recommend a magnetic resonance imaging (MRI) scan to look at the tendons. The MRI scan is a test that uses magnetic waves instead of X-rays. This test shows the tendons and other soft tissues of the body. It can show the damage in the material that makes up the tendon.
In rare cases it is difficult to find the exact source of your pain. In these cases, your doctor may ask you to go through more sophisticated imaging tests. Your doctor may also inject a local anesthetic into the tendon suspected of causing the pain. If the pain goes away, you have found the right tendon.
Treatment
What can be done for the problem?
Tendon problems can be difficult to treat effectively. They can last for many months to several years, even with treatment. You should expect your treatment to take from six to nine months. Even if treatment is effective, your pain may come back. The exact treatment your doctor recommends depends on which tendon is affected.
Your doctor will probably recommend nonsteroidal anti-inflammatory drugs (NSAIDs), such as aspirin and ibuprofen, to help control the inflammation and pain. NSAIDs are usually used for a short time with tendon problems. Your doctor may also suggest ice or heat treatments.
If nothing helps relieve the pain, corticosteroid injections around the tendon are sometimes used. Doctors disagree on whether to use corticosteroid injections in tendons. Even if your doctor does use injections, they are not safe in all cases. Injections into tendons can cause more injury–in some cases, the tendons actually tear. It is generally recommended to give no more than three corticosteroid injections, at least three months apart. Patients need to avoid heavy activity for a few weeks after the injection.
You will need to rest to give your body time to heal. If playing tennis injured your tendon, stop playing tennis until it is completely healed. You should only take part in activities that don’t strain the injured tendon.
Your doctor may refer you to a physical or occupational therapist. A therapist will teach you stretches and exercises to help your tendon heal and regain its strength. A therapist can also assess your work site and athletic equipment and recommend changes to reduce the strain on your tendon. Depending on your type of injury, you may be asked to try such special equipment as arch supports, heel lifts, and splints.
Most people with chronic tendon problems can find ways to relieve the pain and take part in their normal activities, even if the problem doesn’t completely go away. In a few cases, patients can’t find ways to manage the pain even after six months. For these patients, surgery may be necessary. Surgery can be very successful in relieving the pain of chronic tendonitis.